

Copyright 2009-2014 Saviz Inc. All rights reserved.
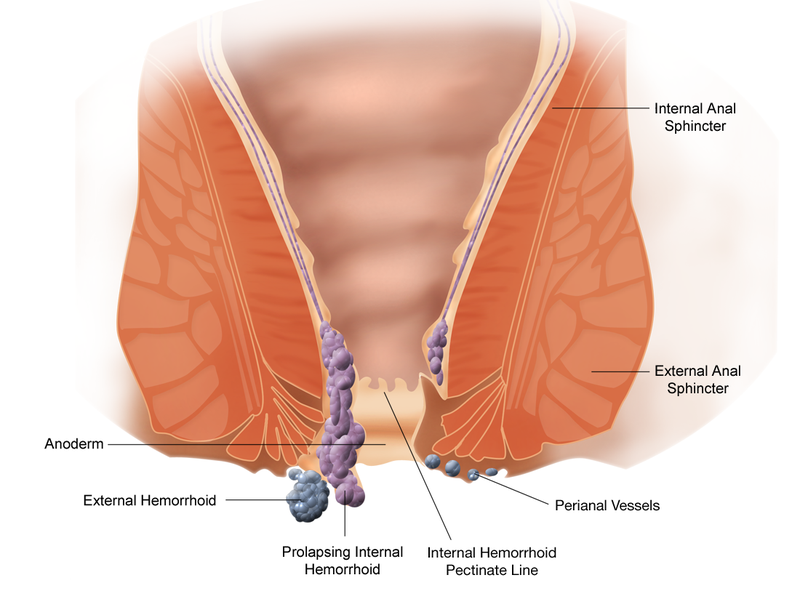
Anal Fissure:
Early, or acute, fissures have the appearance of a simple tear in the anoderm, whereas chronic fissures, defined by symptoms lasting more than 8-12 weeks, are further characterized
by edema and fibrosis. Typical inflammatory manifestations of chronic fissures include a sentinel pile, or skin tag, at the distal fissure margin and a hypertrophied anal papilla proximal to the fissure in the anal canal.
Trauma to the anal canal secondary to the passage of a hard stool is believed to be a common initiating factor. A history of constipation is not universally obtained, however, and some patients report an episode of diarrhea before the onset of symptoms.
The clinical hallmark of an anal fissure is pain during, and particularly after, defecation. In acute fissures, pain may be short-lived, but it can last several hours or even all day in the
presence of a chronic fissure. The pain is frequently described as passing razor blades or glass shards. Understandably, patients with anal fissures may often fear bowel movements.
Rectal bleeding, although not uncommon, is usually limited to minimal bright red blood seen on the toilet tissue.
Fissures may be frequently misdiagnosed as hemorrhoids by primary care providers. The differential diagnosis includes perianal abscess, anal fistula, inflammatory bowel disease,
sexually transmitted disease, tuberculosis, leukemia, and anal carcinoma.
Conservative management
Almost half of all patients diagnosed with an acute fissure will heal with conservative measures, i.e., sitz baths and psyllium fiber supplementation, with or without the addition of topical anesthetics or anti-inflammatory ointments.
Operative Treatment
The primary goal in the treatment of a nonhealing anal fissure is to decrease abnormally elevated resting anal tone.
Operative procedures, such as manual anal dilatation or internal sphincterotomy, have been advocated as initial modes of treatment because they produce permanent reductions in maximum
resting anal pressures.
Lateral Internal Sphincterotomy
The use of internal sphincterotomy in the treatment of anal fissure was introduced by Eisenhammer in the early 1950s.
Medical Management
Sphincter Relaxants
"chemical sphincterotomy," aimed at reducing mean maximum resting anal pressures, without permanent sphincter injury. Preparations have included:
various nitrate formulations, including nitroglycerin (NTG) ointment, glyceryl trinitrate (GTN), and isosorbide dinitrate (ISDN) oral and topical calcium channel blockers, including nifedipine
and diltiazem (DTZ) and botulinum toxin (BT). Botulinum Toxin (BT) is an exotoxin produced by the bacteriumClostridium botulinum. BT injections can be given easily, on an outpatient basis,
and are well tolerated. The commercial availability of BT has prompted several prospective trials examining its efficacy in the treatment of anal fissure
About Fissures
If you have any question or you need additional images, films, articles or etc. please send an Email to info@rasoulazizi.com , I will be glad to help you.
.png)
.jpg)
.jpg)


.jpg)